Every medical supply, procedure, and service billed to Medicare or a private insurer needs a standardized code attached to it. That’s where HCPCS coding comes in. The Healthcare Common Procedure Coding System is the universal language that providers, payers, and suppliers use to communicate exactly what was performed or provided during patient care, and how much should be reimbursed for it.
At Ascend BioGraft, we work with this system daily. Our amniotic tissue allografts, used to treat chronic, non-healing wounds, are reported to Medicare using specific HCPCS Level II codes. When we help clinicians with reimbursement verification and documentation, accurate coding is the foundation that makes coverage possible.
If you’re a healthcare provider, biller, or even a patient trying to understand a claim, knowing how HCPCS works gives you a real advantage. This article breaks down the two levels of HCPCS codes, explains how they differ, and walks through how they’re used in practice to report supplies and services to Medicare and other insurers.
What HCPCS coding is and what it covers
HCPCS stands for the Healthcare Common Procedure Coding System, and it functions as the standardized framework that the U.S. healthcare system uses to report medical procedures, supplies, and services on insurance claims. If you want to understand what is HCPCS coding at its most basic level, think of it as a shared dictionary. Every item or service gets a specific alphanumeric code, and that code tells payers like Medicare exactly what the provider performed or supplied during patient care. Without that shared language, billing across thousands of different providers, insurers, and government programs would be unworkable.
The origin and purpose of HCPCS
The Centers for Medicare & Medicaid Services (CMS) developed and maintains HCPCS to create consistency across all medical billing in the United States. Before a standardized system existed, providers used different terminology to describe the same services, which created confusion, delays, and inconsistencies in reimbursement. CMS introduced HCPCS to solve that problem by assigning a unique code to each distinct service, product, or procedure, giving every party in the billing process a common reference point they could rely on.
CMS updates HCPCS codes on both a quarterly and annual basis, so staying current with code changes is essential for accurate billing and timely reimbursement.
The system is used not just by Medicare but also by Medicaid, private insurers, and workers’ compensation programs across the country. Any payer that processes medical claims in the U.S. almost certainly uses HCPCS codes to review, approve, or deny coverage. That broad adoption is what makes this coding system central to healthcare operations rather than a tool exclusive to government programs.
What types of services and supplies HCPCS covers
HCPCS covers a wide range of items and services. At a high level, it captures everything from physician visits and surgical procedures to durable medical equipment, prosthetics, orthotics, and medical supplies. For wound care specifically, it includes products like amniotic tissue allografts, skin substitutes, and the application procedures tied to them. Those are the codes most directly relevant to providers working with biologic grafts for chronic wound treatment.
The scope of HCPCS extends into less obvious areas as well. You will find codes for transportation services such as ambulance rides, dental procedures, vision care, and hearing devices, among others. The system is broad enough to account for virtually any service or product a provider might deliver to a patient, regardless of the clinical specialty involved.
Here is a quick overview of the major categories HCPCS covers:
- Medical and surgical procedures reported through CPT codes (Level I)
- Durable medical equipment (DME) such as wheelchairs, walkers, and oxygen equipment
- Biologics and skin substitutes including amniotic and placental tissue grafts
- Drugs and biologicals administered in outpatient settings
- Transportation and non-physician services like ambulance and home health visits
- Dental, vision, and hearing services not captured in standard CPT codes
That breadth is what makes HCPCS the backbone of medical billing rather than a niche tool for a single specialty. When you submit a claim for any product or service, HCPCS gives you the precise code to make that claim legible to every payer reviewing it.
HCPCS Level I vs Level II codes
HCPCS is divided into two distinct levels, and understanding the difference between them is fundamental to understanding what is HCPCS coding in practice. Level I and Level II codes serve different purposes, cover different types of services, and are maintained by different organizations. Knowing which level applies to a given service directly affects how you submit a claim and whether it gets paid.

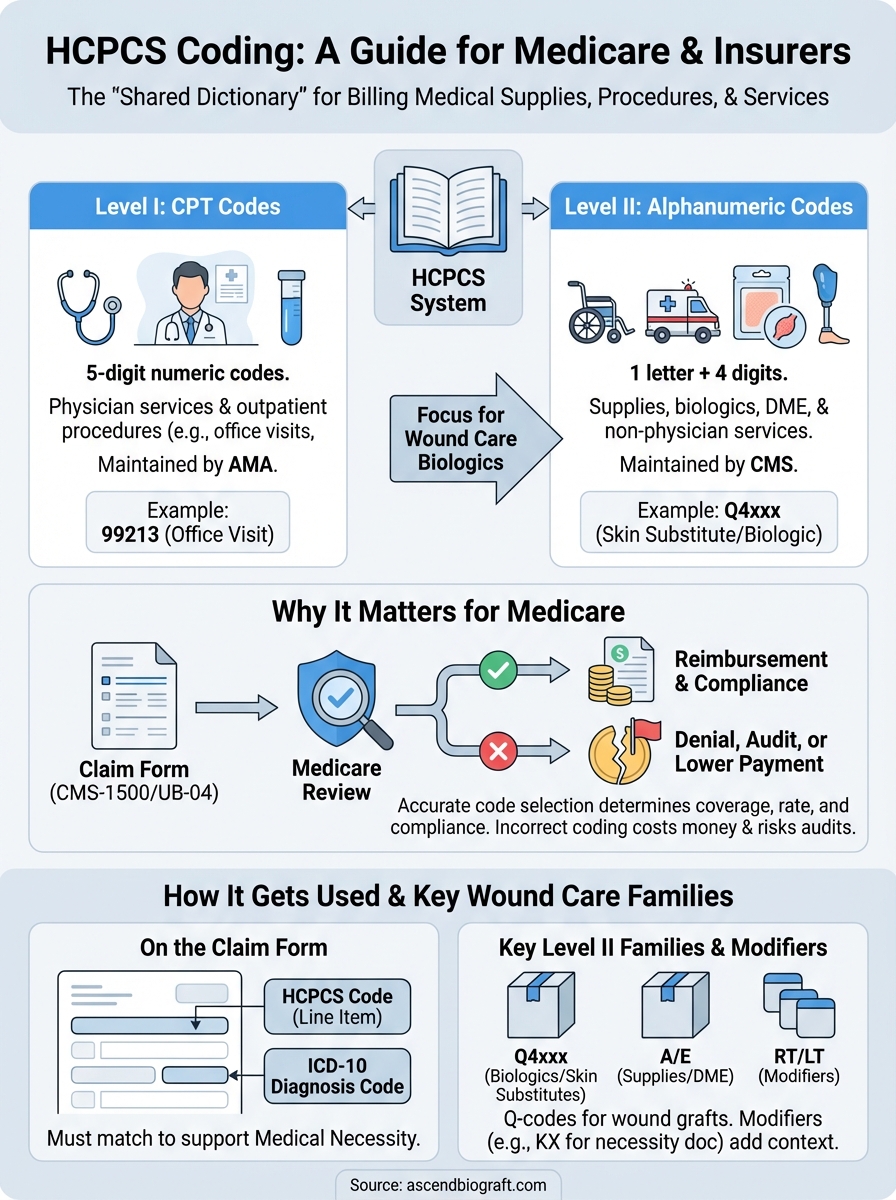
Level I: CPT codes
Level I codes are identical to the Current Procedural Terminology (CPT) codes developed and maintained by the American Medical Association (AMA). These five-digit numeric codes cover the vast majority of physician services and outpatient procedures, including office visits, surgeries, diagnostic tests, and imaging. If a provider performs a procedure in a clinical setting, it almost certainly gets reported with a Level I CPT code.
Because the AMA owns and updates CPT codes annually, providers must use the current code set each year to avoid claim denials based on outdated codes.
CPT codes are procedure-focused by design, meaning they describe what a clinician did rather than what product was supplied to the patient. They form the foundation of most clinical billing but leave significant gaps when it comes to supplies, equipment, and services that fall outside a physician’s direct procedural work.
Level II: Alphanumeric codes
Level II codes fill the gap that CPT codes leave behind. CMS maintains these codes and uses them to cover products, supplies, and services that CPT codes do not address, including durable medical equipment, ambulance transportation, and biologic wound care products like amniotic tissue allografts. These codes follow an alphanumeric format: one letter followed by four digits (for example, Q4xxx codes commonly used for skin substitutes and grafts).
Providers billing for non-physician services or advanced wound care biologics rely on Level II codes more than any other part of the system. When Ascend BioGraft helps clinicians navigate reimbursement for amniotic tissue grafts, the applicable Level II codes are central to that process. Getting these codes right determines whether Medicare approves the claim or flags it for incorrect coding, which is why accurate code selection matters before you ever submit a claim.
Why HCPCS matters in Medicare billing
Medicare does not accept vague descriptions of care. When a provider submits a claim, every service and product on that claim must correspond to a valid HCPCS code. Without the correct code, Medicare has no way to determine coverage eligibility, calculate reimbursement rates, or verify medical necessity. That is why understanding what is HCPCS coding is not optional for anyone billing into the Medicare program.
HCPCS as Medicare’s required billing language
Medicare Part B covers a broad range of outpatient services, physician procedures, and medical supplies, and it uses HCPCS codes as the primary mechanism to identify and price each item on a claim. When you submit a claim for durable medical equipment, a biologic wound graft, or an infused drug, Medicare looks up the submitted code to determine the applicable fee schedule rate and coverage rules for that specific item. No code means no payment. The wrong code can trigger a denial, an audit, or a demand for repayment if the error is caught post-payment.
Medicare processes billions of claims each year, and the HCPCS code you select is the single most important data point on any claim for supplies or non-physician services.
How coding accuracy directly affects reimbursement
Incorrect coding costs providers money in two directions. If you submit a code that does not match the product you supplied, Medicare may deny the claim outright or pay at a lower rate. On the other side, overcoding, meaning selecting a code that describes a more expensive item than what you actually provided, creates compliance risk and potential liability under the False Claims Act.
For wound care providers specifically, biologic graft codes under the Q4xxx family carry strict documentation requirements tied to wound size, tissue type, and medical necessity. If the code you select does not align with the documentation in the patient record, Medicare can recoup the payment during a post-payment review. Getting the right code from the start, supported by accurate records, is the only reliable path to consistent reimbursement.
How HCPCS codes get used on a claim
When you submit a claim to Medicare or a private insurer, HCPCS codes appear as individual line items on a standardized claim form. Each line identifies a specific service or product, the corresponding code, the units provided, and the date of service. Understanding what is HCPCS coding in a practical billing context means knowing exactly where these codes sit on a claim and what supporting data must accompany them for the claim to process correctly.
The claim forms that carry HCPCS codes
Two primary forms handle the majority of medical claims in the United States. The CMS-1500 is used by physicians, non-physician practitioners, and outpatient suppliers to bill professional services. The UB-04 (CMS-1450) is used by hospitals and facilities to bill institutional services. Both forms include dedicated fields for HCPCS codes, and both require that each code be paired with the appropriate ICD-10 diagnosis code to establish medical necessity before Medicare will consider the claim payable.
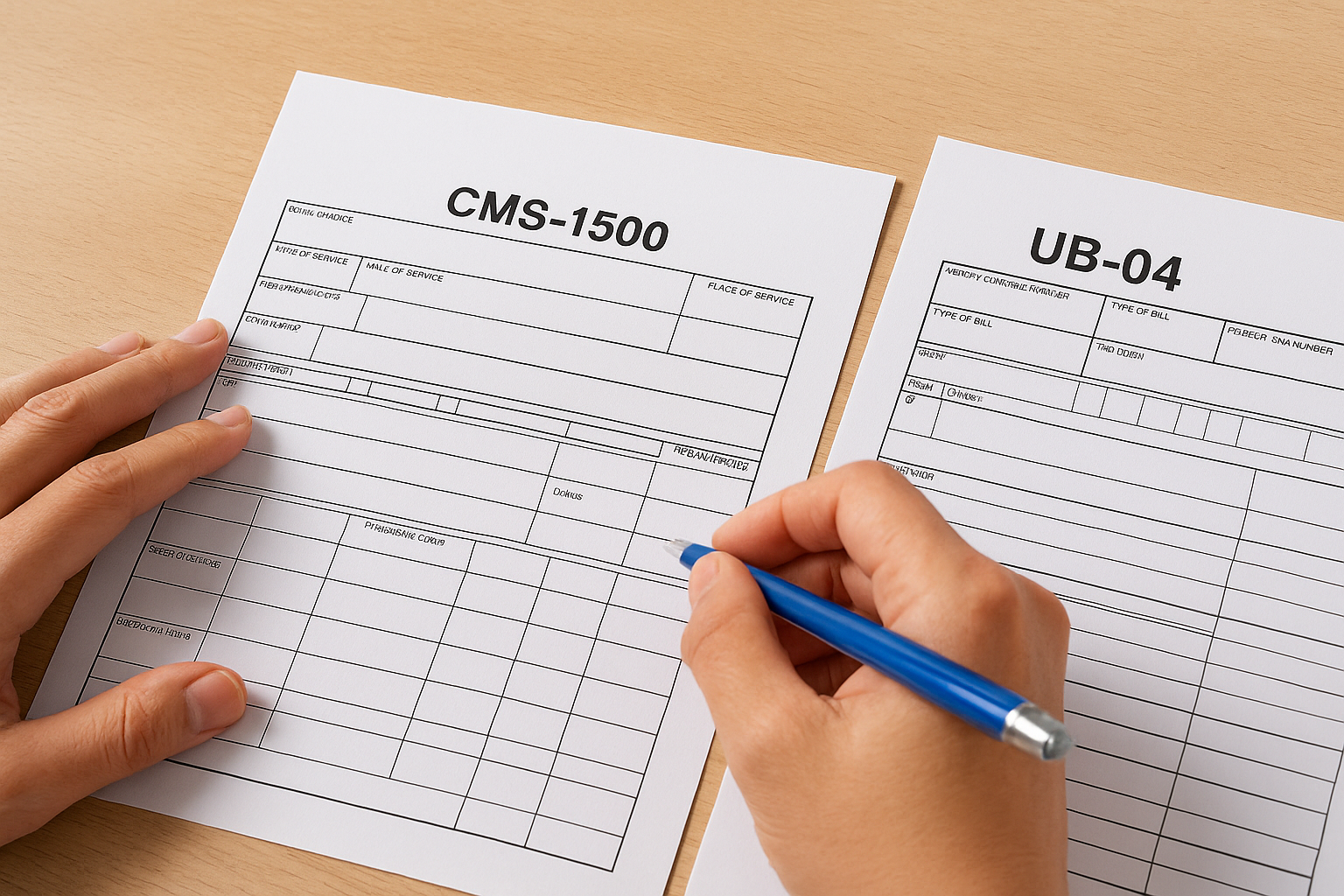

The diagnosis codes you pair with your HCPCS codes must directly support medical necessity, or Medicare will deny the claim regardless of whether the HCPCS code itself is correct.
What happens after you submit the code
Once Medicare receives your claim, its systems cross-reference the submitted HCPCS code against its coverage policies to confirm the item or service qualifies as a covered benefit. If the code clears that check, Medicare applies the applicable fee schedule rate and calculates the reimbursement amount. If the code fails, Medicare returns a remittance advice explaining the denial reason, which you then use to correct and resubmit the claim within the allowed timeframe.
For wound care providers billing biologic grafts, this process requires that the units submitted match the actual tissue size applied to the patient. Medicare defines specific billing units for skin substitute codes, and submitting the wrong unit count is one of the most common reasons claims for advanced wound care products get denied or reduced in payment. Accurate measurement documentation at the time of application protects your reimbursement before a claim ever reaches the payer’s desk.
Common HCPCS code families and modifiers
When you work through what is HCPCS coding in a billing context, the sheer number of available codes can feel overwhelming. In practice, most providers within a given specialty use a small cluster of code families on a regular basis. Knowing which families apply to your work, and how modifiers refine those codes, keeps your claims accurate and your denials low.
Key Level II code families
Level II codes are organized by their starting letter, and each letter or letter range maps to a general category of services or products. Here are the families most relevant to wound care and related medical services:
| Code Family | What It Covers |
|---|---|
| A codes | Medical and surgical supplies, dressings, wound care accessories |
| E codes | Durable medical equipment including beds, wheelchairs, and support surfaces |
| G codes | Procedures and professional services not classified in CPT |
| Q codes | Temporary codes including skin substitutes and biologic grafts |
| L codes | Orthotic and prosthetic devices |
For wound care providers, Q4xxx codes are the most consequential. Medicare uses this family to cover amniotic tissue allografts, skin substitutes, and other advanced biologics, and each specific product typically has its own assigned Q code tied to application size and tissue type.
Selecting the correct Q code for a biologic graft requires matching the code to the exact tissue product applied, not just the general category of wound care biologics.
HCPCS modifiers
Modifiers are two-character additions appended to a base HCPCS code to provide Medicare with additional context about how or where a service was delivered. Common modifiers include RT and LT to indicate the right or left side of the body, GY to signal that an item is not covered by Medicare, and KX to confirm that the provider has documentation on file supporting medical necessity.
Your choice of modifier can mean the difference between a paid claim and a denial. Using modifier KX on a wound graft claim, for example, signals to Medicare that you have medical necessity documentation ready, which directly supports timely reimbursement without a payer reaching out to request records after submission.
Key takeaways and next steps
Understanding what is HCPCS coding gives you a practical foundation for cleaner claims, faster reimbursement, and fewer denials. Level I CPT codes cover physician procedures, while Level II alphanumeric codes cover supplies, biologics, and services outside that scope. Medicare requires both accurate codes and supporting documentation before it will process any payment. For wound care providers, selecting the right Q4xxx code and pairing it with correct diagnosis codes and modifier usage directly determines whether your claim clears or gets denied.
Every step in the billing process builds on accurate code selection. If you work with advanced wound care biologics like amniotic tissue allografts, having a knowledgeable partner on reimbursement verification and documentation makes the process significantly more manageable. Explore Ascend BioGraft’s wound care solutions to see how we support clinicians with rapid insurance verification and the clinical documentation needed to back every claim you submit.

