Every chronic wound that refuses to close has an underlying story, and often, part of that story involves nutritional deficiency. Among all micronutrients studied in wound repair, the relationship between vitamin C and wound healing stands out as one of the most well-documented in clinical literature. Without adequate vitamin C, your body simply cannot produce the collagen needed to rebuild damaged tissue.
For the millions of Americans managing diabetic ulcers, surgical wounds, or other non-healing injuries, understanding this connection isn’t academic, it’s practical. Vitamin C deficiency impairs every phase of wound healing, from the initial inflammatory response to the final remodeling of new tissue. Clinicians and patients alike benefit from knowing how this essential nutrient works at the cellular level, what the research actually shows, and how much is enough to support recovery.
At Ascend BioGraft, we provide advanced amniotic tissue allografts that give chronic wounds the biological scaffold they need to heal. But even the most effective graft performs best in a body equipped with the right building blocks. That’s why we believe patient education on nutritional factors like vitamin C is inseparable from quality wound care. This article breaks down the mechanisms behind vitamin C’s role in tissue repair, examines the clinical evidence for supplementation, covers recommended dosages, and explains how proper nutrition works alongside advanced biologics to help wounds finally close.
Why vitamin C matters for wound repair
Your body treats every wound as an emergency, triggering a cascade of biological processes that depend on specific nutrients to work correctly. Vitamin C (ascorbic acid) sits at the center of several of these processes, making it one of the few micronutrients that directly influences wound repair outcomes. When your vitamin C levels fall below optimal ranges, your body lacks the chemical raw materials to rebuild damaged tissue efficiently, and healing stalls at predictable points in the repair sequence.
Collagen synthesis: the structural foundation
Collagen is the most abundant protein in your body, and it forms the primary structural framework of healing tissue. Vitamin C acts as a required cofactor for two enzymes, prolyl hydroxylase and lysyl hydroxylase, that stabilize collagen molecules during synthesis. Without adequate vitamin C, these enzymes cannot function properly, and your body produces structurally weak collagen that breaks down faster than it forms.
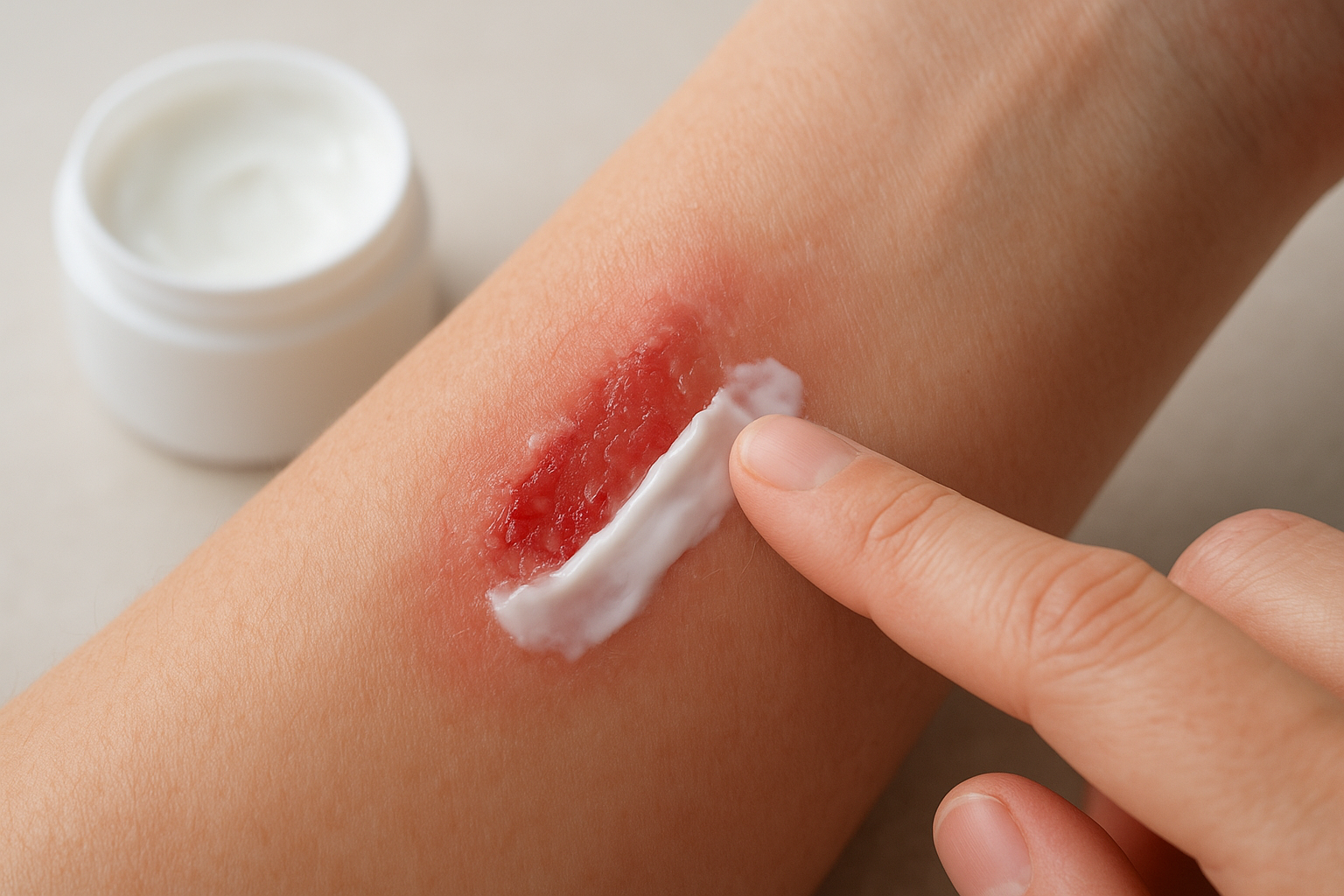
Deficient collagen synthesis doesn’t just slow wound closure; it can cause already-healed wounds to reopen, a phenomenon documented in both classic scurvy cases and modern clinical observations of depleted patients.
This is precisely why the relationship between vitamin c and wound healing runs deeper than general nutrition. Collagen isn’t just part of healing, it is the scaffold on which new tissue forms. Fibroblasts, the cells responsible for depositing collagen into wound beds, cannot perform this function effectively without a consistent and sufficient supply of ascorbic acid to drive the enzymatic reactions involved.
Inflammation control and immune response
Wound healing begins with inflammation, which is a controlled biological response that clears debris and pathogens from the injury site. Vitamin C directly supports neutrophils and macrophages, the white blood cells that drive this early-stage cleanup. These immune cells actively accumulate vitamin C at concentrations far above what circulates in blood plasma, which indicates that your immune system requires high local concentrations to function at full capacity in and around wound tissue.
Your body also relies on vitamin C to regulate oxidative stress at the wound site. Healing tissue generates reactive oxygen species as a byproduct of immune activity. Vitamin C neutralizes these molecules before they damage healthy surrounding cells, keeping the inflammatory phase productive rather than destructive. Without this buffering effect, prolonged oxidative stress can block the transition from inflammation into the proliferative phase, where new tissue actually forms.
Angiogenesis and tissue oxygenation
New blood vessel formation, known as angiogenesis, is essential for delivering oxygen and nutrients to healing tissue. Vitamin C plays a measurable role in stimulating the vascular endothelial growth factor (VEGF) pathways that drive this process. Without adequate blood vessel growth into the wound bed, even well-supported tissue will lack the oxygen it needs to complete repair and transition into mature scar formation.
Chronic wounds, particularly diabetic foot ulcers and venous leg ulcers, frequently show impaired angiogenesis as a contributing factor to delayed healing. This is one reason why a patient’s nutritional status, including circulating vitamin C levels, matters so much in complicated wound cases. A wound bed that lacks new vasculature stays hypoxic, and hypoxic tissue heals slowly regardless of what other interventions you apply at the surface.
Why deficiency is more common than most clinicians expect
Vitamin C deficiency is not limited to malnourished populations. Hospitalized patients, surgical recovery patients, and individuals with chronic illnesses frequently show low plasma ascorbate levels even when their diets appear adequate. Stress, infection, and systemic inflammation all accelerate vitamin C consumption, meaning your body burns through its reserves faster precisely when healing demands are highest.
Standard dietary intake may not replenish these reserves quickly enough during acute or prolonged healing episodes. Recognizing this gap is the first step toward addressing it as part of a comprehensive wound care strategy rather than leaving it as an afterthought once clinical interventions are already underway.
How vitamin C supports healing in the body
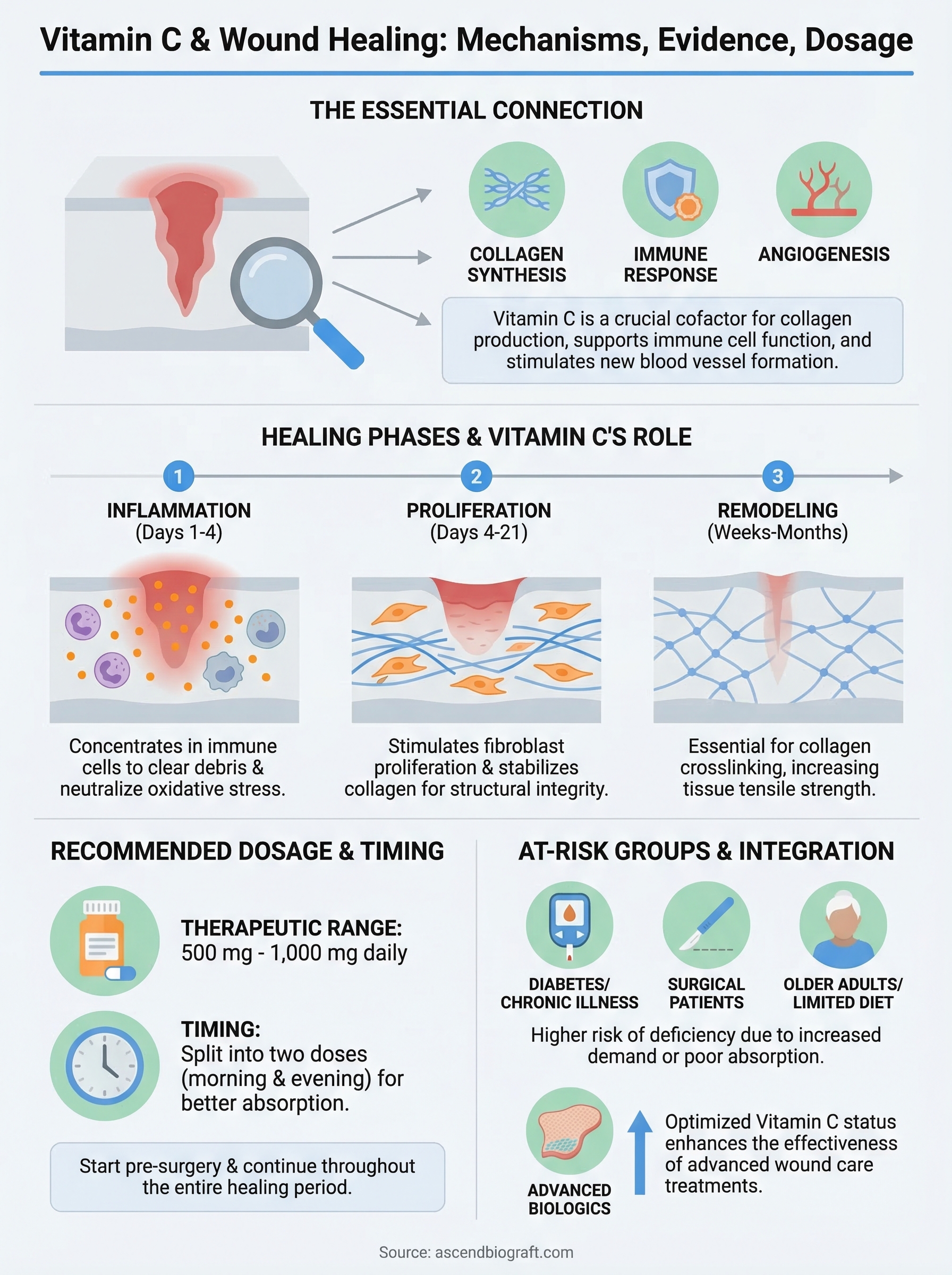
Your body doesn’t heal wounds in one continuous flow. It moves through three distinct phases: inflammation, proliferation, and remodeling. Vitamin C participates actively in all three, making it one of the only nutrients with a documented role at every stage of the repair sequence. Understanding where it acts helps explain why deficiency disrupts healing so completely rather than just slowing it in a single area.
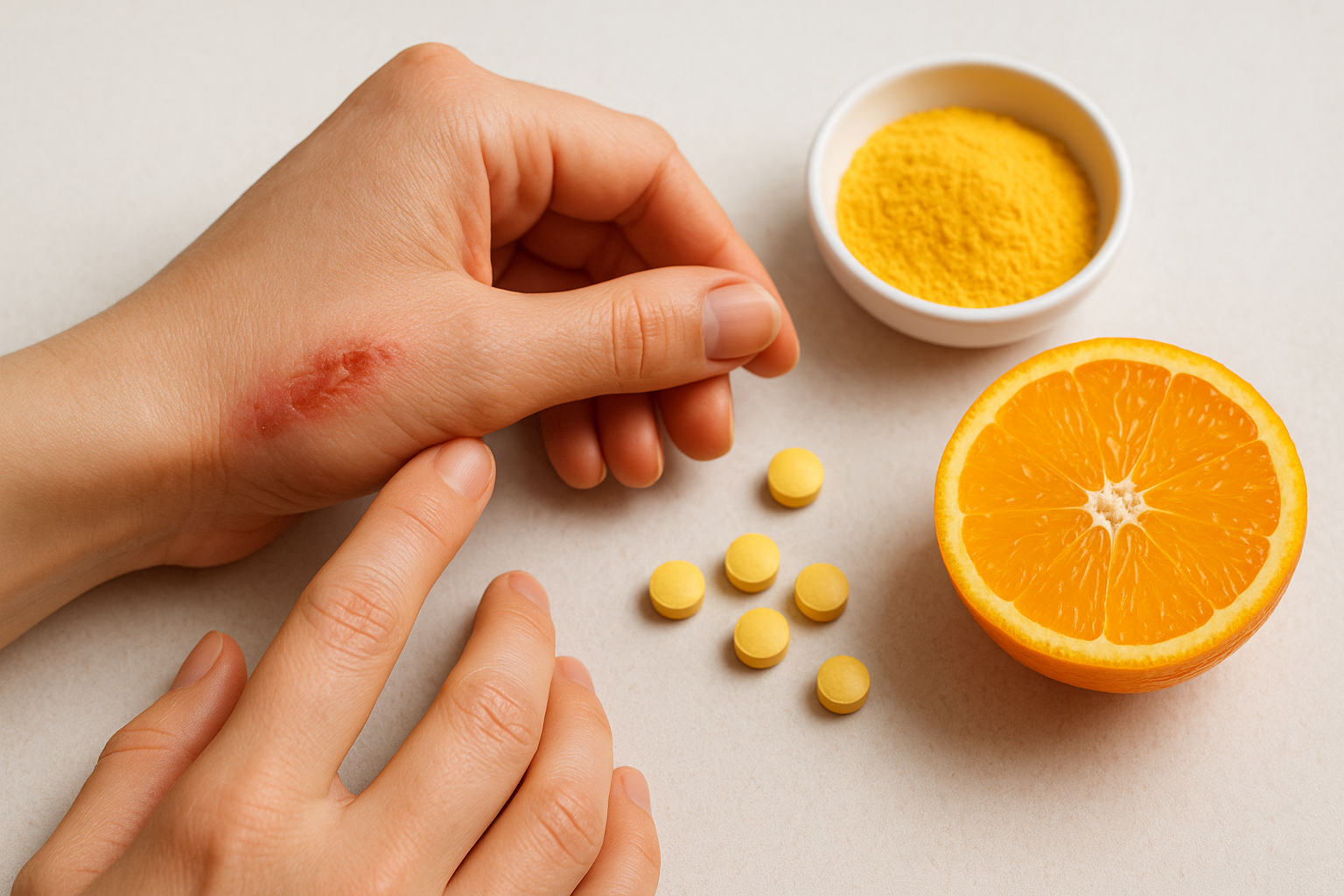
Ascorbate accumulation at the wound site
When tissue gets damaged, neutrophils and macrophages actively concentrate vitamin C inside themselves to levels 20 to 100 times higher than normal plasma concentrations. This isn’t passive absorption. It’s a selective, energy-driven process that signals just how dependent immune function is on high local ascorbate availability.
When your circulating vitamin C levels fall below threshold, this accumulation process breaks down, and your immune cells lose a significant portion of their capacity to clear debris and pathogens from the wound bed.
These same cells use ascorbate to neutralize reactive oxygen species generated as a byproduct of their own activity. Without this buffering, oxidative byproducts accumulate and damage the healthy tissue forming around the wound edge. Vitamin C acts as a direct electron donor to neutralize these molecules before they spread, protecting the new tissue your body is working to build.
Fibroblast function and extracellular matrix assembly
Fibroblasts are the primary cells responsible for filling a wound with new structural tissue. Vitamin C directly stimulates fibroblast proliferation, increasing the number of cells available to deposit collagen and other matrix proteins into the wound bed. Without sufficient ascorbate, fibroblast activity slows, and your body falls behind in its ability to close the wound with organized tissue.
Beyond cell count, vitamin C regulates the quality of the extracellular matrix these fibroblasts produce. Collagen crosslinking, the process that gives mature scar tissue its tensile strength, depends on hydroxylation reactions that require ascorbate as a cofactor. When crosslinking is incomplete, the resulting tissue tears under normal mechanical stress, which is a particularly serious problem in high-load areas like the plantar surface of the foot.
The connection between vitamin c and wound healing at this cellular level explains why even subclinical deficiencies translate into measurable delays in wound closure. A patient doesn’t need to develop full scurvy for their healing capacity to drop significantly. Plasma ascorbate levels that simply sit in the low-normal range are enough to blunt fibroblast output, impair collagen quality, and leave wounds stalled at stages they should have already moved through.
What the clinical evidence shows
Research on vitamin C and wound healing spans decades, and the findings consistently point in one direction: adequate ascorbate levels correlate with faster wound closure and better tissue outcomes, while deficiency measurably slows repair across multiple wound types. Clinical studies have moved beyond confirming that vitamin C matters to examining how much it matters, in which patient populations, and under what conditions your patients are most at risk.
Studies on surgical and acute wounds
Several controlled trials have examined vitamin C supplementation in surgical patients, where the timing and conditions of tissue damage are well-defined. Research reviewed by the National Institutes of Health found that patients receiving supplemental ascorbate after surgery showed reduced rates of wound complications compared to those receiving standard care alone. The benefit appeared most pronounced in patients who entered the procedure with below-average baseline ascorbate levels, a group that is larger than most clinicians anticipate.
Patients undergoing major surgery can deplete plasma vitamin C by more than 50% within the first 24 hours post-operation, making supplementation in the recovery window a clinically relevant consideration.
Burn wound studies have also produced consistent findings. Burn injuries cause a massive spike in oxidative stress and inflammatory activity, both of which accelerate vitamin C consumption. Trials using high-dose intravenous ascorbate in burn patients have shown reductions in fluid resuscitation requirements, smaller wound surface areas at follow-up, and shorter hospitalization times, suggesting that restoring vitamin C status rapidly after acute injury changes the trajectory of repair.
Evidence in chronic wound populations
Chronic wound patients present a different challenge because nutritional depletion builds gradually rather than occurring as a single acute event. Studies examining patients with diabetic foot ulcers, pressure injuries, and venous leg ulcers consistently find that a disproportionate share carry low or deficient plasma ascorbate levels, often without any clinical signs obvious enough to trigger routine screening.
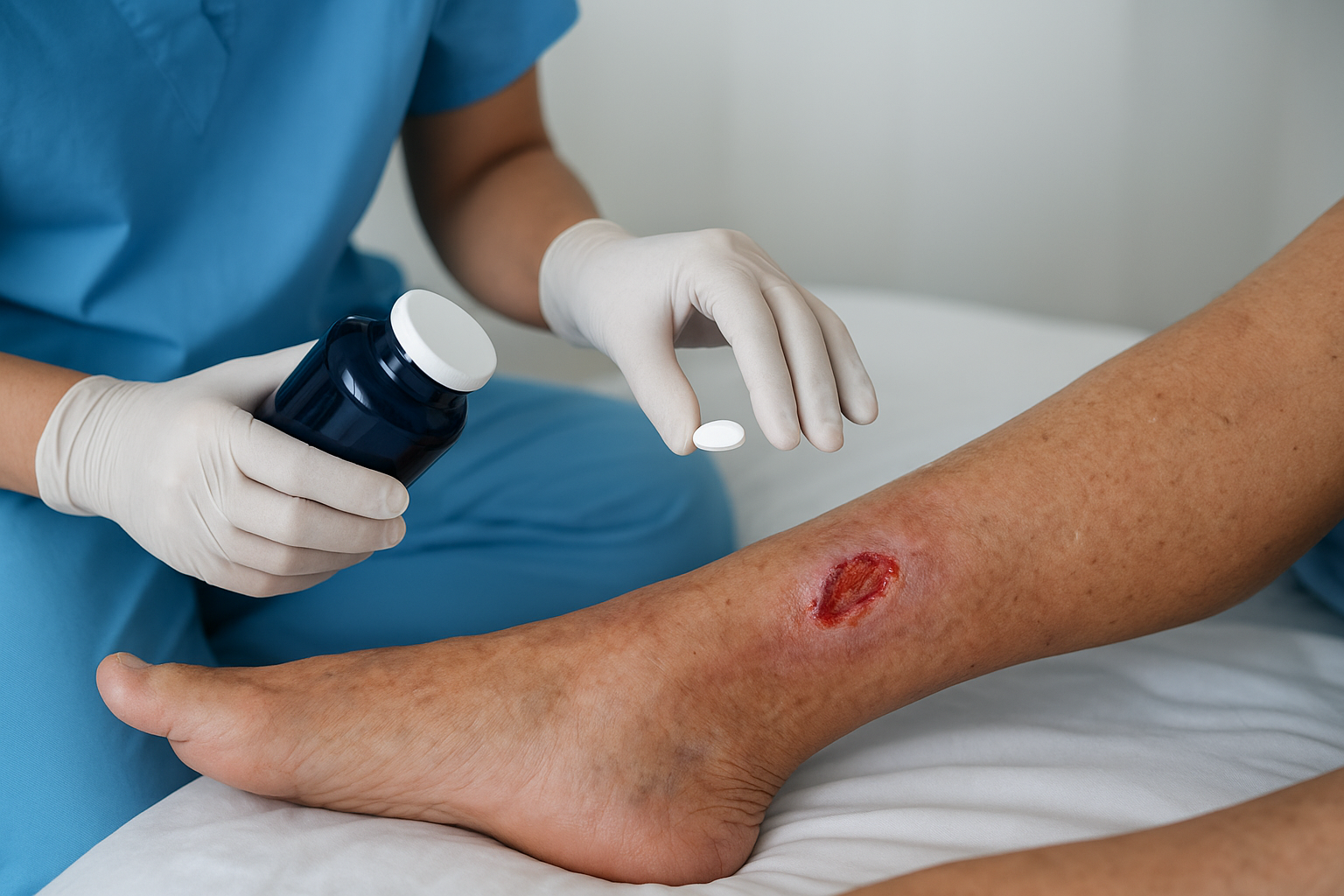
Supplementation trials in chronic wound populations have shown meaningful improvements in healing rates when vitamin C is added to standard care protocols. One analysis found that patients with pressure ulcers who received ascorbate supplementation demonstrated significantly faster wound surface area reduction compared to placebo groups. Your patients in this population reflect both the nutritional demands of prolonged repair and the baseline deficiency many carry into treatment.
Taken together, the clinical evidence supports treating vitamin C status as a routine assessment point in wound care rather than an optional consideration reserved for patients who appear obviously malnourished.
Dosage and timing for wound healing support
No single dose fits every patient, but research on vitamin C and wound healing gives clear signals about what ranges produce measurable benefits and what falls short. The standard US Recommended Dietary Allowance (RDA) for vitamin C is 75 to 90 mg per day for healthy adults, but this figure is designed to prevent deficiency in otherwise well people, not to meet the elevated demands of active tissue repair.
Therapeutic ranges supported by research
During active wound healing, your body consumes vitamin C at a much faster rate than baseline. Clinical evidence points to a supplementation range of 500 mg to 1,000 mg per day as a meaningful therapeutic target for patients managing surgical recovery or chronic wounds. Some studies in burn and critical care settings have used significantly higher doses through intravenous delivery, but those protocols fall outside standard outpatient wound care for most patients.

For patients receiving outpatient wound care, a daily oral supplement of 500 mg to 1,000 mg represents a practical and well-tolerated range that aligns with what the research supports.
Divided dosing across two intakes per day improves absorption because your intestinal transport system for ascorbate saturates at higher single doses. Rather than taking 1,000 mg at once, splitting into two 500 mg doses taken morning and evening allows your body to absorb a greater proportion of each dose and maintain more consistent plasma levels throughout the day.
When to start and how long to continue
Timing matters as much as dose. Starting supplementation before a planned surgical procedure gives your body time to build adequate reserves before tissue stress begins. For elective surgeries, two to four weeks of pre-operative supplementation can help ensure your plasma ascorbate levels enter the recovery period at a higher baseline rather than already depleted.
For chronic wound patients, supplementation should continue throughout the entire active healing period rather than stopping once the wound starts closing. Tissue remodeling, the final phase of repair where new collagen matures and strengthens, continues for weeks to months after visible surface closure. Your body’s demand for ascorbate doesn’t drop to baseline simply because the wound looks intact from the outside.
Reassessing your patient’s nutritional status at regular follow-up visits helps you identify whether supplementation is achieving its intended effect or whether underlying absorption issues are limiting the benefit. Gastrointestinal conditions, medication interactions, and metabolic factors all affect how much ascorbate your patient actually retains, making periodic review a practical part of the care plan rather than a one-time recommendation.
Food sources vs supplements
Getting enough vitamin C from diet alone sounds straightforward, but the reality for patients managing active wounds is that food sources and supplements serve different roles in reaching therapeutic ascorbate levels. Understanding which approach fits your situation helps you build a realistic plan rather than assuming that a daily glass of orange juice covers your needs during recovery.
Getting vitamin C from food
Whole foods remain the best baseline source of ascorbic acid for maintaining healthy vitamin C status in well people. Citrus fruits, bell peppers, strawberries, broccoli, and kiwi all deliver meaningful amounts per serving, and eating a varied diet that includes several of these regularly keeps most healthy adults above deficiency thresholds. The table below shows approximate vitamin C content for common high-ascorbate foods:
| Food | Serving Size | Approximate Vitamin C |
|---|---|---|
| Red bell pepper | 1 cup, raw | 190 mg |
| Kiwi | 1 medium | 70 mg |
| Orange | 1 medium | 70 mg |
| Strawberries | 1 cup | 85 mg |
| Broccoli | 1 cup, cooked | 80 mg |
Cooking reduces vitamin C content significantly, with boiling cutting levels by up to 50%. Steaming or eating these foods raw preserves more of the ascorbate content, making preparation method a practical consideration if you are relying primarily on diet to meet your daily intake.
Why supplements make more sense during active healing
Food alone rarely delivers the 500 mg to 1,000 mg per day that research supports for active wound healing. Reaching 1,000 mg through diet would require eating roughly five to six cups of raw red bell pepper daily, which is neither practical nor sustainable for most patients. This gap is exactly where targeted supplementation fills the shortfall that diet cannot reasonably close.
When your body is actively repairing tissue, its demand for vitamin C exceeds what a normal diet can supply, making supplementation a clinical decision rather than just a personal wellness choice.
Ascorbic acid supplements are widely available, inexpensive, and well-absorbed when taken in divided doses. Buffered forms, such as calcium ascorbate or sodium ascorbate, reduce gastrointestinal discomfort in patients who find plain ascorbic acid irritating at higher doses, giving you a practical option for sensitive patients without requiring a prescription.
The connection between vitamin c and wound healing means your supplementation strategy should match the intensity of your healing demands, not simply mirror what a healthy person needs to stay above deficiency.
Who may need extra vitamin C
Not every patient enters wound care with the same nutritional baseline. While vitamin C deficiency can affect anyone under sufficient physical stress, certain groups face a consistently higher risk of running low precisely when their bodies need the most support. Recognizing which patients fall into these categories lets you address nutritional gaps as part of the care plan rather than discovering them after healing has already stalled.
Patients with diabetes or chronic illness
People managing diabetes, kidney disease, or other chronic systemic conditions tend to run lower vitamin C levels than the general population. Elevated oxidative stress from chronically high blood glucose accelerates ascorbate consumption, meaning a diabetic patient’s baseline stores deplete faster even without an active wound. When you add a diabetic foot ulcer or venous leg ulcer to the picture, the body’s demand for ascorbate surges at a point when reserves are already compromised.
The connection between vitamin C and wound healing is especially relevant for diabetic patients, since both impaired immune function and slowed collagen synthesis compound the healing difficulties that high blood glucose already creates.
Patients on hemodialysis face a related problem. Dialysis sessions remove water-soluble vitamins including ascorbate directly from circulation, and dietary restrictions common in kidney disease limit the ability to replenish through food alone. These patients benefit from routine nutritional monitoring and targeted supplementation as standard practice.
People recovering from surgery or serious injury
Surgical patients deplete their plasma vitamin C levels dramatically in the first 24 to 48 hours post-operation, and critically ill patients in intensive care settings often show near-deficient levels within days of admission. Your post-surgical patients entering recovery with average or below-average baseline stores can cross into functional deficiency before standard dietary intake has any chance to compensate.
Burn patients represent an extreme version of this dynamic. Massive injury triggers acute phase responses that consume ascorbate rapidly, and fluid shifts associated with major burns further dilute circulating levels. In these cases, waiting for dietary sources to catch up is not a viable strategy.
Older adults and those with limited diets
Aging reduces gastrointestinal absorption efficiency and frequently coincides with reduced dietary variety, making older adults disproportionately likely to carry suboptimal vitamin C levels into wound care. Patients in long-term care facilities or with limited mobility often have restricted access to fresh produce, which means their food-based intake falls well short of even baseline maintenance needs, let alone the elevated demands of active tissue repair.
Safety, side effects, and drug interactions
Vitamin C is one of the safer supplements in clinical use, but safety and risk-free are not the same thing. Understanding where the boundaries sit helps you use supplementation confidently within a wound care plan without creating new problems while addressing a nutritional gap. The established tolerable upper intake level set by the National Institutes of Health is 2,000 mg per day for adults, and most therapeutic protocols for wound healing fall comfortably below that ceiling.
Common side effects at higher doses
Most people tolerate oral vitamin C doses up to 1,000 mg per day without noticeable side effects. Above that level, gastrointestinal symptoms become the most frequently reported issue. Your digestive tract absorbs ascorbate through a saturable transport mechanism, meaning that what your intestines cannot absorb stays in the gut and draws in water, which produces the symptoms most commonly associated with excessive intake.
Splitting your daily dose into two smaller servings reduces the amount your gut must process at once, which significantly lowers the likelihood of gastrointestinal discomfort without requiring you to reduce your total daily intake.
The side effects most commonly reported at higher doses include:
- Loose stools or diarrhea
- Nausea and stomach cramping
- Heartburn or acid reflux in susceptible individuals
- Headache at very high single doses
Buffered formulations like calcium ascorbate reduce acidity and are better tolerated in patients who experience reflux or gastric sensitivity with plain ascorbic acid. Switching formulation rather than cutting dose keeps your patient on a therapeutic level without discomfort driving non-compliance.
Drug interactions to be aware of
The relationship between vitamin C and wound healing includes a less-discussed dimension around drug interactions. Ascorbate affects how several medications are absorbed, metabolized, or tested in the body, which makes a brief medication review a practical step before adding supplementation to a wound care plan. Patients taking blood thinners such as warfarin should be monitored carefully, as high-dose vitamin C has been reported to interfere with anticoagulation stability in some individuals, though the effect is inconsistent across patients.
Ascorbate at higher doses can also affect the accuracy of certain lab tests, including glucose monitors that use older electrochemical methods, which is a relevant concern for your diabetic patients who track blood sugar daily. Vitamin C can also increase iron absorption, which benefits most wound patients but requires caution in patients with hemochromatosis or other iron metabolism disorders. Flagging these interactions at the outset of supplementation prevents complications that are easy to avoid with basic awareness.
How vitamin C fits into wound care plans
Vitamin C and wound healing belong in the same clinical conversation, but in practice, nutritional status often gets treated as a separate issue from the wound care protocol itself. Integrating ascorbate assessment and supplementation directly into your care plan closes this gap and gives every other intervention you apply a better environment to work in.
Making nutritional assessment part of your intake process
Adding a brief nutritional screen at the start of wound care lets you identify vitamin C deficiency before it becomes an obstacle to progress. You don’t need extensive lab panels for every patient. A focused intake review covering dietary habits, chronic illness status, recent surgery, and current medications surfaces most of the high-risk patients described in earlier sections. For patients who screen as likely deficient, plasma ascorbate testing confirms the picture and gives you a measurable baseline to track against.
Catching a nutritional deficit at intake rather than six weeks into a stalled healing course changes your ability to act on it while it still meaningfully affects outcomes.
Documenting nutritional status alongside wound measurements also creates a more complete clinical record. When a wound isn’t progressing as expected, having baseline ascorbate data in the chart gives you actionable information rather than forcing you to rule out nutritional factors retroactively.
Combining vitamin C with advanced wound care interventions
Biologic treatments, including amniotic tissue allografts, create the structural and biological conditions that a wound bed needs to close. These grafts deliver growth factors, extracellular matrix components, and cellular signals that drive tissue regeneration. However, the cells receiving those signals still depend on adequate ascorbate to carry out collagen synthesis and support the immune response that clears debris and allows new tissue to mature.
Treating vitamin c and wound healing as complementary rather than competing priorities means you get the most out of both approaches. A patient whose plasma vitamin C levels are optimized responds to biologic treatment with better fibroblast activity, stronger collagen deposition, and more effective angiogenesis than one who is nutritionally depleted when the graft is applied.
Practical integration looks like this: confirm nutritional status at intake, start supplementation where indicated, apply your advanced wound care protocol, and reassess both the wound and the patient’s nutritional status at each follow-up. This cycle keeps nutritional support active throughout the full repair timeline rather than treating it as a one-time checkbox. When every layer of the care plan is working together, you give your patient the most direct path to a closed, stable wound.
Key takeaways
The connection between vitamin C and wound healing runs through every phase of tissue repair. Your body needs ascorbate to synthesize stable collagen, support immune cell function, control oxidative stress, and drive the angiogenesis that keeps healing tissue oxygenated. Deficiency disrupts all of these processes simultaneously, which is why low ascorbate levels translate directly into stalled wounds and poor tissue outcomes.
Therapeutic supplementation in the range of 500 mg to 1,000 mg per day, split into two doses, gives most wound care patients a practical and well-tolerated way to close the gap between what diet supplies and what active repair demands. Patients with diabetes, older adults, post-surgical patients, and anyone under sustained physiological stress carry the highest risk of running low at exactly the wrong time.
Advanced biologics perform best in a body that has the raw materials to respond. If you want to learn how amniotic tissue allografts can support your patients’ healing, contact the Ascend BioGraft team today.

