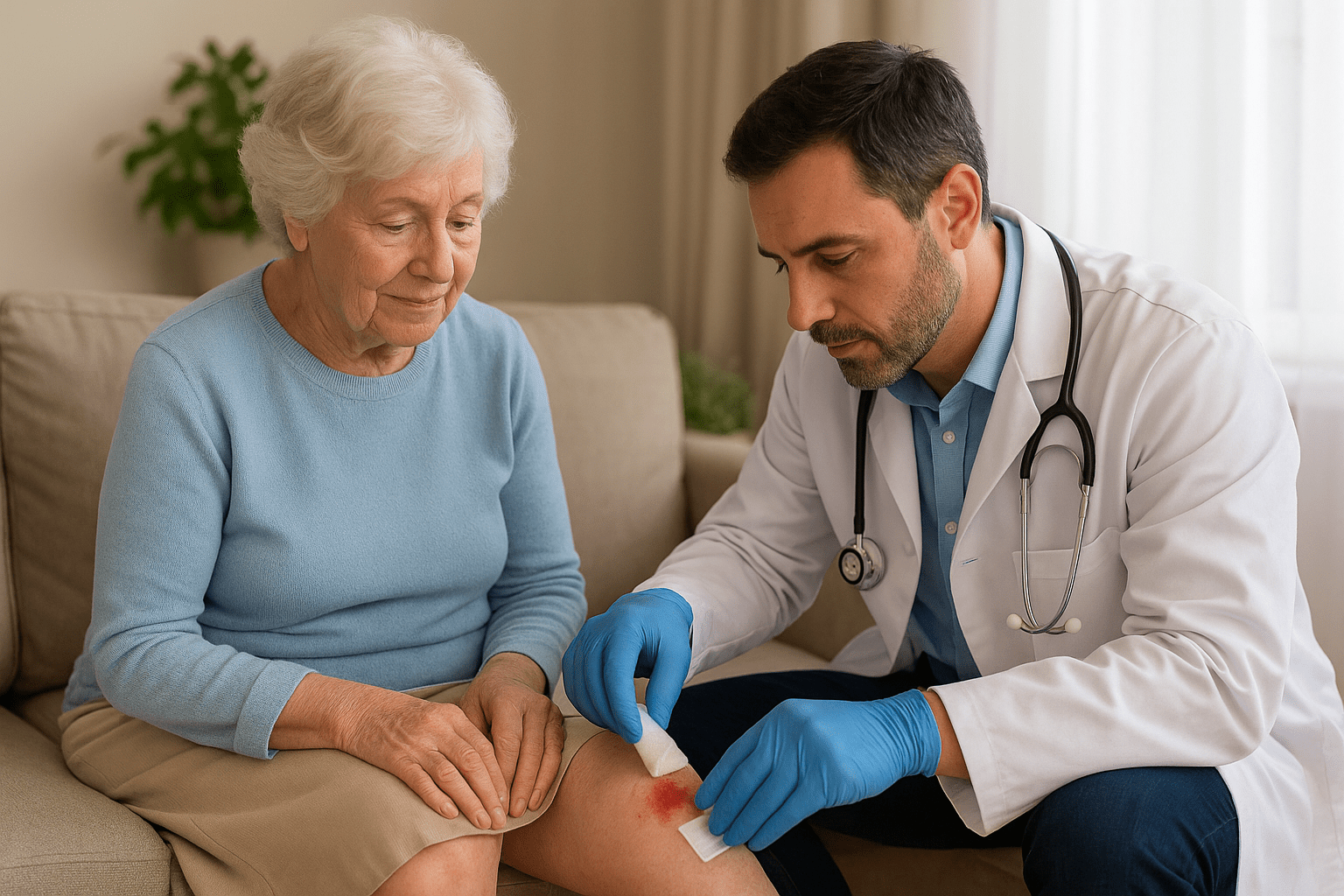
When a chronic wound refuses to heal and getting to a clinic feels impossible, physician house calls wound care Philadelphia services offer a practical solution. For patients recovering at home, in skilled nursing facilities, or hospice settings, traveling to appointments creates real barriers, from mobility challenges to transportation logistics that can delay critical treatment. That’s where mobile wound care changes the equation. Instead of asking patients to come to the doctor, a licensed physician arrives at the bedside with the expertise and tools needed to treat complex wounds on-site. This model delivers specialist-level care where patients actually live, closing the gap between hospital discharge and full recovery. At Philadelphia Wound Care, we provide exactly this type of service, physician-led house calls focused on diabetic ulcers, pressure wounds, vascular ulcers, and post-surgical complications. This article breaks down what mobile wound care involves, who benefits most, and what to expect when scheduling a visit. What physician house call wound care means Physician house call wound care means a licensed doctor travels to your location to evaluate and treat wounds that aren’t healing properly. Instead of scheduling appointments at a medical office, the physician brings clinical expertise and medical equipment directly to your bedside, whether that’s your private home, a skilled nursing facility, or an assisted living residence. This approach removes transportation barriers while maintaining the same level of medical oversight you’d receive in a hospital wound clinic. The core difference from clinic visits Traditional wound care requires you to physically visit a specialized facility, often multiple times per week. With physician house calls wound care Philadelphia services, the specialist comes to you with everything needed to perform comprehensive wound assessments, apply advanced dressings, and administer therapies that promote healing. This model eliminates travel stress and ensures patients with limited mobility still receive expert medical attention without risking their stability or comfort. Mobile wound care brings the same clinical standards of a hospital wound center to the patient’s environment, not a downgraded version of treatment. The physician examines your wound in the setting where you spend most of your time, which often reveals environmental or care factors that wouldn’t be visible in a clinic. Your treatment plan adapts to your actual living conditions, making recommendations more practical and easier to follow between visits. Who qualifies as the physician For mobile wound care to meet medical standards, a board-certified physician must lead the treatment, not just a nurse or wound care specialist working independently. In Philadelphia Wound Care’s model, a licensed General Surgeon conducts each house call, bringing surgical training and advanced wound management experience to every patient encounter. This physician-led approach ensures you receive diagnostic accuracy and treatment decisions backed by full medical authority, including the ability to prescribe medications, order imaging, or coordinate with your primary care team. Why physician-led in-home wound care helps Having a physician manage your wound care at home means you receive medical decisions from someone with full diagnostic authority, not just wound observations. A physician can prescribe medications, order diagnostic tests, adjust treatment protocols, and recognize systemic health issues that affect healing, all during the same visit. This level of clinical oversight prevents complications from escalating into emergency situations that require hospitalization. Physician-led house calls give you the same treatment authority as a hospital wound clinic without leaving your residence. When a board-certified doctor leads your care, your treatment plan adapts immediately based on medical judgment, not protocol checklists that need supervisor approval. The physician coordinates directly with your primary care team and specialists, ensuring everyone involved in your recovery works from the same clinical picture. For patients with complex conditions like diabetes or vascular disease, this integrated approach catches problems before they become critical. Direct medical authority at your bedside Physician house calls wound care Philadelphia services deliver full medical decision-making in real time, eliminating the delays that happen when nurses must consult off-site doctors. Your physician can adjust wound debridement techniques, prescribe antibiotics for emerging infections, or initiate advanced therapies during the visit. This immediate response prevents minor setbacks from becoming major complications that extend your recovery timeline. How an in-home wound care visit works When you schedule physician house calls wound care Philadelphia services, the process begins with a simple phone consultation to understand your wound type and current treatment history. Your care team gathers basic medical information and coordinates with your referring physician or facility staff to ensure everyone stays aligned on your treatment plan. Scheduling typically happens within 24 hours of your initial contact, with arrival times confirmed by phone the day before your appointment. What happens during the physician visit The physician arrives at your location with portable medical equipment and wound care supplies needed for a complete evaluation. Your doctor performs a thorough wound assessment, measuring dimensions, checking for signs of infection, and documenting your wound’s healing progress with clinical photography. Based on this examination, the physician explains your treatment options, applies appropriate dressings or therapies, and adjusts your care plan as needed. Mobile wound care visits include the same comprehensive evaluation you’d receive in a hospital wound center, just performed where you live. Coordination after your visit Before leaving, your physician schedules your next appointment and provides clear instructions for wound maintenance between visits. The medical team submits detailed visit notes to your primary care doctor and coordinates directly with facility nurses if you live in a skilled nursing or assisted living setting. This ensures your wound care continues seamlessly even when the physician isn’t physically present. Services and advanced therapies you can get at home Mobile wound care delivers more than basic dressing changes at your bedside. Physician house calls wound care Philadelphia services include surgical debridement, infection management, and advanced regenerative treatments that typically require specialist appointments at hospital wound centers. Your physician brings the clinical capabilities to perform these procedures safely in your home environment, maintaining the same sterile protocols used in medical facilities. Wound debridement and surgical care During your house call, the physician can perform surgical debridement to remove dead tissue that prevents healing. This procedure requires medical training to execute safely, which is why physician-led services differ from nurse-only wound care. Your doctor also handles infection control through wound cultures, antibiotic selection, and monitoring for complications that could require hospitalization. Advanced wound procedures performed at
Top 5 Home Health Wound Care Physicians In Philadelphia
When a wound refuses to heal, getting to a clinic can feel like an obstacle course, especially for patients recovering from surgery, managing diabetes, or dealing with limited mobility. That’s where a home health wound care physician Philadelphia families can trust becomes essential. Having a qualified specialist come directly to your home or care facility removes transportation barriers and brings advanced medical treatment to your bedside. Finding the right provider matters more than you might expect. Wound care isn’t one-size-fits-all, and the difference between a nurse-led visit and physician-led oversight can significantly impact healing outcomes. Whether you’re caring for a parent with a stubborn pressure ulcer or managing your own post-surgical wound, you need a provider who offers specialized expertise, not just routine check-ins. The good news is that Medicare and most major insurers now cover many of these in-home services, making quality care more accessible than ever. This guide highlights five reputable home health wound care physicians serving the Philadelphia area, including our own team at Philadelphia Wound Care. We’ve compiled this list to help you compare options, understand what each practice offers, and make an informed decision about who will manage your wound healing journey. Each provider brings something different to the table, so let’s look at what sets them apart. 1. Philadelphia Wound Care, LLC Philadelphia Wound Care operates as a physician-led mobile practice that brings specialist-level treatment directly to your location. Instead of sending a nurse practitioner, this practice dispatches a board-certified General Surgeon to perform all evaluations and treatments at your bedside. That distinction matters when you’re dealing with complex wounds that haven’t responded to standard care protocols. What they treat and advanced therapies offered The practice handles the full spectrum of chronic wound types, including diabetic ulcers, pressure sores, venous insufficiency wounds, and post-surgical complications. What sets their treatment apart is the use of allograft and regenerative therapies that accelerate healing in wounds that have stalled for weeks or months. These advanced biologics work by providing a scaffold for new tissue growth, something standard dressings cannot accomplish. How the mobile physician visit works You schedule a visit through their direct line or referral from your hospital case manager. The surgeon arrives at your home, nursing facility, or hospice setting with all necessary equipment and supplies. During the visit, you receive a complete wound assessment, debridement if needed, and application of appropriate dressings or biologics. Follow-up schedules depend on your wound’s progress, not arbitrary calendar intervals. Who this option fits best This service works best for homebound patients with wounds that require physician expertise rather than basic nursing care. Family caregivers who struggle to transport elderly parents find this model eliminates the stress of clinic visits while maintaining high-quality medical oversight. Referral, scheduling, and turnaround times You can initiate care through a physician referral or direct contact with the practice. Philadelphia Wound Care commits to a 24-hour response window for urgent cases, which beats the typical three-to-five-day wait at traditional clinics. Their streamlined intake process means less paperwork between you and treatment. “The 24-hour response commitment ensures your wound gets expert attention before complications worsen.” Insurance coverage and expected costs Medicare Part B covers the physician visits and advanced biologics without requiring prior authorization in most cases. Medicare Advantage plans and major commercial insurers also provide coverage, though you should verify your specific benefits. The practice handles billing directly, so you avoid upfront payment for covered services. 2. Kane Wound Care Kane Wound Care provides specialized wound treatment through a team that includes certified wound specialists and coordinating physicians who work alongside your existing healthcare providers. The practice focuses on delivering consistent protocols across multiple care environments, making it easier to maintain treatment continuity as your recovery progresses. Their approach emphasizes collaboration rather than replacing your primary medical team. Clinical team and scope of wound care Your care comes from certified wound care specialists who follow physician-directed protocols. The team handles diabetic foot ulcers, surgical wounds, and pressure injuries using evidence-based dressing protocols and infection management. While they don’t perform advanced biologics applications onsite, they coordinate these interventions through referring physicians when needed. Care settings and how treatment is delivered Kane operates primarily within skilled nursing facilities and assisted living communities throughout the Philadelphia region. Their specialists conduct scheduled visits to assess wounds, change dressings, and document progress. You receive treatment in your facility room rather than transferring to an outside clinic. Who this option fits best This service works well for facility residents who need consistent wound monitoring but not necessarily physician-level oversight at every visit. Patients managing less complex wounds with stable conditions typically benefit from their structured visit schedule. Referral requirements and coordination with other clinicians Your facility’s medical director initiates the referral, and Kane’s team coordinates directly with your attending physician for treatment orders. They provide detailed documentation to all involved clinicians, ensuring everyone stays informed about wound progression. “Coordinated documentation keeps your entire care team aligned on treatment progress and necessary adjustments.” Insurance coverage and expected costs Medicare Part B covers wound care specialist visits when ordered by a physician. Most Medicare Advantage and commercial insurance plans also provide coverage, though facility contracts may affect your specific arrangement. 3. Ascend BioGraft Ascend BioGraft specializes in regenerative wound therapies delivered directly to your home, focusing specifically on wounds that haven’t responded to conventional treatment approaches. Their model centers on applying advanced skin grafts and bioengineered tissue products rather than standard dressing changes. You work with a team trained in biologics application who coordinate closely with your referring physician to determine which graft technology suits your specific wound type. What they treat and graft-based options The practice targets diabetic foot ulcers, venous leg ulcers, and pressure injuries that have plateaued despite weeks of standard care. Their graft options include amniotic membrane products and bioengineered skin substitutes that provide cellular scaffolding for new tissue growth. These applications typically occur during scheduled home visits rather than requiring clinic transfers. In-home care model and service area Ascend operates throughout Philadelphia and surrounding counties, bringing necessary supplies and equipment to your location. Their specialists perform wound preparation, graft application, and post-application monitoring during bedside visits. Follow-up assessments happen at intervals determined by your wound’s response to treatment. Who this option fits best This service
11 Best Snacks Diabetics Can Eat for Steady Blood Sugar
Managing blood sugar isn’t just about what you eat at mealtimes, it’s also about what happens between them. For people with diabetes, choosing the best snacks diabetics can rely on makes a real difference in maintaining steady glucose levels throughout the day. Smart snacking prevents dangerous spikes and crashes, supports energy, and plays a direct role in overall health outcomes, including how well your body heals. At Philadelphia Wound Care, we see firsthand how blood sugar control affects wound healing in diabetic patients. Chronically elevated glucose impairs circulation and slows tissue repair, which is why dietary choices matter far beyond the dinner table. The snacks you reach for can either support your recovery or work against it. This guide covers 11 satisfying, blood-sugar-friendly snacks that won’t derail your glucose levels. Whether you’re managing diabetes at home or supporting a loved one’s care, these options offer practical solutions you can use starting today. https://youtu.be/GKCQb2hTWA4 1. Hard-boiled eggs Hard-boiled eggs are one of the best snacks diabetics can keep on hand because they deliver complete protein without any carbohydrates. You get six grams of protein per egg along with healthy fats that slow digestion and prevent blood sugar spikes. They’re portable, inexpensive, and require zero prep beyond boiling, which makes them practical for anyone managing diabetes at home or on the go. Why it helps keep blood sugar steady Eggs contain zero carbs, which means they won’t raise your blood glucose on their own. The protein and fat work together to stabilize your levels after eating, especially if you pair them with a small amount of whole-grain bread or vegetables. Research shows that protein slows the absorption of any carbohydrates you eat alongside it, giving you more control over post-snack glucose readings. Protein from eggs also supports tissue repair, which is particularly important for diabetic patients dealing with slow-healing wounds. How to make it more filling If one or two eggs don’t satisfy you, add non-starchy vegetables like cherry tomatoes, bell pepper strips, or cucumber slices on the side. You can also sprinkle everything bagel seasoning or smoked paprika on top for flavor without adding sugar or carbs. Another option is to slice the eggs over a small bed of leafy greens with a splash of vinegar for a mini salad that feels more substantial. Portion and carb notes A single large hard-boiled egg has 78 calories and less than one gram of carbohydrates, making it easy to fit into most meal plans. Most people with diabetes can comfortably eat one to two eggs as a snack without worrying about glucose changes. If you’re watching cholesterol, talk to your doctor, but recent guidance suggests that dietary cholesterol from eggs has less impact on blood levels than previously thought for most individuals. Best times to eat it Hard-boiled eggs work well as a mid-morning or mid-afternoon snack when you need to bridge the gap between meals. They’re also effective before bed if you experience overnight blood sugar dips, since the protein provides steady fuel without spiking glucose. Keep a batch in your fridge so you always have a grab-and-go option ready when hunger hits. 2. Plain Greek yogurt with berries Plain Greek yogurt paired with berries gives you a protein-rich snack that satisfies your sweet tooth without causing blood sugar chaos. Greek yogurt contains twice the protein of regular yogurt, which slows digestion and helps prevent glucose spikes. Fresh berries add natural sweetness, fiber, and antioxidants while keeping total carbs manageable, making this combination one of the best snacks diabetics can build in under two minutes. Why it helps keep blood sugar steady Greek yogurt delivers around 15 to 20 grams of protein per serving, which blunts the blood sugar impact of the carbohydrates in berries. The live cultures in yogurt may also improve gut health and insulin sensitivity over time, though you’ll feel the immediate benefit of sustained energy. Berries rank low on the glycemic index compared to other fruits, so they won’t spike your glucose the way bananas or grapes might. Choosing unsweetened Greek yogurt gives you full control over how much natural or artificial sweetener you add, if any. How to build it without added sugar Start with plain, full-fat or low-fat Greek yogurt and check the label to confirm it has zero added sugars. Add a half cup of fresh or frozen berries like strawberries, blueberries, or raspberries for natural sweetness. You can sprinkle cinnamon or vanilla extract for extra flavor without carbs, or stir in a small amount of stevia if you want it sweeter. Portion and carb notes A standard serving is one cup of Greek yogurt with around half a cup of berries, which typically gives you 15 to 20 grams of carbohydrates total. That amount fits comfortably into most diabetic meal plans and keeps your snack under 150 calories when you choose low-fat yogurt. Measure your portions at first so you know what satisfies you without overdoing the carbs. Best times to eat it This snack works well in the morning or early afternoon when you need energy that lasts. The protein makes it effective after exercise to support muscle recovery without raising blood sugar too quickly. You can also eat it as a light dessert alternative when you want something sweet without the guilt or glucose spike. 3. Nuts and seeds Nuts and seeds rank among the best snacks diabetics can reach for when you need lasting energy without blood sugar spikes. They pack healthy fats, protein, and fiber into a portable package that requires zero preparation. A small handful delivers the nutrients your body needs to maintain stable glucose levels between meals, and the variety available means you won’t get bored rotating your options. Why it helps keep blood sugar steady Nuts and seeds contain minimal carbohydrates compared to their fat and protein content, which keeps your blood sugar from jumping after you eat. The monounsaturated and polyunsaturated fats slow digestion and help your body absorb nutrients more gradually. Studies show that people who eat nuts regularly often have better long-term blood sugar control than those who avoid them, likely because the combination of nutrients supports insulin sensitivity. The fiber in nuts also feeds beneficial gut bacteria, which may improve how your body processes glucose over time. Best picks and what to limit Almonds, walnuts, pistachios, and pumpkin seeds give you the most nutritional value with the least impact on blood
Non-Healing Wounds Philadelphia: When To Seek Specialist Care
A wound that refuses to heal after several weeks isn’t just frustrating, it’s a warning sign. When standard treatments fail and that stubborn ulcer or surgical site remains open, the risk of infection, tissue damage, and serious complications climbs rapidly. For patients dealing with non-healing wounds Philadelphia offers specialized care options, but knowing when to seek help makes all the difference in outcomes. Chronic wounds affect millions of Americans, with diabetic ulcers, pressure sores, and vascular wounds being among the most common culprits. Many patients assume these wounds will eventually close on their own or that their primary care provider can manage them indefinitely. Unfortunately, delayed specialist intervention often leads to preventable hospitalizations and, in severe cases, amputations. Philadelphia Wound Care brings physician-led wound management directly to patients at home, in skilled nursing facilities, and hospice settings, eliminating the transportation barriers that keep many from accessing the advanced care they need. This article explains when a wound crosses from “slow to heal” to “needs a specialist,” what treatment options exist in the Philadelphia area, and how to take the next step toward recovery. What counts as a non-healing wound https://youtu.be/dVJyyA-jFGg Medical professionals use a four-week benchmark to separate normal healing from chronic wound territory. If your wound hasn’t shown significant progress after four weeks of appropriate care, it qualifies as non-healing. Progress means the wound is closing, showing healthy tissue growth, and reducing in size, not simply staying stable or getting worse. Timeline markers that signal trouble You should watch for specific warning signs during the healing process. A wound that stalls at the same size for two weeks despite proper treatment deserves attention. Wounds that initially improve but then stop progressing also fit the non-healing category, as do those that develop new complications like increased drainage or worsening tissue quality. A wound that hasn’t reduced in size by at least 20-40% after two weeks of treatment likely needs specialist intervention. The location matters too. Pressure ulcers on heels or sacrum, diabetic foot ulcers, and venous leg ulcers tend to heal more slowly than surface cuts or abrasions because of compromised blood flow and constant pressure on the affected area. These wounds demand specialized attention from the start rather than waiting the full four weeks. Common types of chronic wounds Several wound categories routinely become chronic problems. Diabetic ulcers account for a large percentage of non healing wounds Philadelphia specialists treat, typically appearing on feet and lower legs where nerve damage masks pain and poor circulation slows healing. Pressure sores develop when skin breaks down from sustained pressure, most often affecting bedridden or wheelchair-bound patients. Surgical wounds that reopen or drain continuously beyond the expected recovery period also qualify as non-healing. Arterial and venous ulcers result from circulation problems that starve tissue of oxygen and nutrients needed for repair. Why wounds fail to heal Your body’s healing process relies on adequate blood flow, proper nutrition, and a functioning immune system to close wounds efficiently. When one or more of these elements breaks down, the wound stalls in its tracks. Understanding why your wound refuses to heal helps you identify which underlying factors need addressing before any treatment can work effectively. Medical conditions that interfere Diabetes disrupts healing by damaging blood vessels and nerves, reducing your body’s ability to deliver oxygen and nutrients to the wound site. Your elevated blood sugar levels also weaken immune function, making it harder to fight off infection. Peripheral artery disease restricts blood flow to your extremities, starving tissues of the resources they need to repair themselves. Poor circulation cuts off the oxygen supply that healing tissue depends on, turning minor wounds into major medical problems. Chronic venous insufficiency causes blood to pool in your legs, creating pressure that prevents proper wound closure. Autoimmune conditions and kidney disease further compromise your body’s natural repair mechanisms, while certain medications like steroids slow down tissue regeneration. External factors You can’t heal properly when your wound faces repeated pressure or friction throughout the day. Moisture from sweat or drainage creates an environment where bacteria thrive, while inadequate protein intake deprives your body of the building blocks it needs for tissue repair. When to seek specialist care in Philadelphia You need specialist intervention the moment your wound shows signs of infection or deterioration rather than waiting for the arbitrary four-week mark. Redness spreading beyond the wound edges, increasing pain, foul-smelling drainage, or fever all indicate your body is losing the battle against bacteria. Early specialist involvement prevents minor complications from escalating into hospitalizations or limb-threatening infections. Signs that demand immediate specialist attention Call a wound specialist if you notice darkening tissue, exposed bone or tendon, or a wound that rapidly expands despite treatment. Patients with diabetes should seek help even sooner because nerve damage masks pain that would normally alert you to worsening problems. Wounds that develop thick, hard edges or produce excessive drainage beyond two weeks also warrant specialist evaluation. Waiting to see if a wound improves on its own wastes precious healing time and increases your risk of permanent damage. Philadelphia residents benefit from mobile wound care services that eliminate transportation barriers to specialized treatment. For patients managing non healing wounds Philadelphia offers physician-led care that comes directly to your home or facility, making it easier to get expert evaluation without the physical strain of traveling to a clinic. What a wound specialist does at a visit Your first visit with a wound specialist begins with a thorough examination of your wound and the surrounding tissue. The physician measures wound dimensions, assesses tissue quality, checks for signs of infection, and photographs the area to track healing progress over time. They also review your medical history, current medications, and any underlying conditions that might interfere with healing. What happens during the initial assessment The specialist evaluates your circulation and sensation in the affected area, particularly important for patients dealing with diabetes or vascular disease. They test blood flow using physical examination techniques and may order additional tests if circulation problems appear to be blocking healing. Your wound gets debrided during this visit if dead tissue needs removal. A complete assessment identifies all the factors preventing your wound from closing, not just the visible damage on the surface. Documentation and care planning Your specialist documents wound measurements, tissue types, drainage characteristics, and photographs at every visit to
5 Wound Care Referral Options In Philadelphia For Seniors
Finding the right wound care referral Philadelphia providers can feel overwhelming, especially when you’re managing a loved one’s health or dealing with mobility challenges. Chronic wounds like diabetic ulcers, pressure sores, and venous ulcers require specialized treatment, and knowing your options makes all the difference in recovery outcomes. The good news? Seniors in the Philadelphia area have access to several pathways for expert wound care, from hospital-based clinics to mobile physician services that come directly to your home. Some options require a formal referral from your primary care doctor, while others, like Philadelphia Wound Care, offer streamlined processes that get treatment started faster. This guide breaks down five wound care referral options available to seniors in the Philadelphia region. Whether you’re a caregiver, facility administrator, or patient, you’ll find practical information to help you choose the right fit for your situation. 1. Philadelphia Wound Care house-call wound team Philadelphia Wound Care operates as a mobile medical practice that brings physician-led wound treatment directly to your home, skilled nursing facility, or assisted living community. Unlike traditional wound care clinics that require multiple trips and waiting rooms, this service sends a licensed General Surgeon to your bedside to evaluate and treat complex wounds where you already feel comfortable and safe. What care you can get at home You receive specialized treatment for diabetic ulcers, pressure ulcers, venous ulcers, and post-surgical wounds without leaving your home. The medical team provides advanced therapies including allograft and regenerative treatments that many patients assume are only available in hospital settings. These therapies are covered under Medicare Part B, which removes the financial barrier that often prevents seniors from accessing cutting-edge wound care. How the referral process works Philadelphia Wound Care offers a streamlined referral system that gets you care within 24 hours of receiving a request. Your primary care doctor, hospital case manager, or facility staff can submit a referral directly, or you can contact the practice yourself if you need urgent evaluation. This approach eliminates the long waits that often delay healing when you’re dealing with a chronic wound. The 24-hour response commitment means you don’t spend weeks waiting while a wound worsens. Who this option fits best This service works best for homebound seniors or those with limited mobility who find traveling to appointments physically difficult or impossible. You’ll benefit most if you’re managing complex wounds that haven’t responded to standard treatment or if you need coordination between multiple healthcare providers. Insurance and cost basics for seniors Philadelphia Wound Care accepts Medicare, Medicare Advantage, and major commercial insurance plans. The practice handles direct billing, so you don’t need to file claims yourself or pay upfront for services. What to have ready before the first visit Gather your insurance cards, current medication list, and any recent wound care records from hospitals or previous providers. Having these documents ready helps the physician create a complete treatment plan during the first visit. 2. Penn Wound Care Center Penn Medicine operates a dedicated wound care facility located at Pennsylvania Hospital in Center City Philadelphia. This hospital-based clinic provides comprehensive outpatient treatment for patients dealing with wounds that haven’t healed through standard care, offering both diagnostic services and advanced therapies in a clinical setting. What services the center provides The center treats pressure sores, diabetic foot ulcers, venous ulcers, and surgical wounds that have become complicated. You’ll receive wound debridement, specialized dressings, and hyperbaric oxygen therapy when appropriate for your condition. How to get a referral and schedule You need a formal referral from your primary care physician or specialist to access Penn Wound Care Center. Your doctor’s office submits the referral through Penn’s system, and the scheduling team contacts you within several business days to book your first appointment. Getting your referral submitted early prevents delays in starting treatment. Who this option fits best This option works best for ambulatory seniors who can travel to Center City and manage multiple clinic visits. You should feel comfortable with traditional medical appointments and have reliable transportation to and from the facility. Insurance and cost basics for seniors Penn accepts Medicare, Medicare Advantage, and most major insurance plans. Check your copay requirements before your first visit, as outpatient specialty services typically carry higher copays than primary care visits. What to bring and what to expect at check-in Bring your insurance cards, photo ID, complete medication list, and any imaging results related to your wound. Plan to arrive 15 minutes early for registration and paperwork during your first visit. 3. Jefferson Health wound care and chronic wound services Jefferson Health runs multiple wound care locations across the Philadelphia region, including their main Center City facility and satellite clinics in Northeast Philadelphia and the suburbs. This network approach gives you more flexibility in choosing a location that reduces your travel time while still accessing the same quality of specialized care. What services the center provides Jefferson treats diabetic ulcers, pressure injuries, arterial wounds, and radiation-related tissue damage. The team provides debridement, compression therapy, specialized dressings, and vascular studies to diagnose circulation problems that slow healing. You’ll work with wound care specialists who coordinate with your other doctors to address underlying health issues affecting recovery. How to get a referral and schedule Your primary care doctor submits a referral through Jefferson’s electronic system, which typically processes within three to five business days. The scheduling team calls you to arrange your first appointment at the location most convenient for your situation. Who this option fits best You’ll benefit most from Jefferson if you prefer staying within an established healthcare system where your records already exist. This option works well for seniors who value continuity and want their wound care team to communicate directly with their existing Jefferson providers. Insurance and cost basics for seniors Jefferson accepts Medicare, Medicare Advantage, and most commercial insurance plans. Contact your specific clinic location before your first visit to verify your plan’s coverage and understand any copay responsibilities. How to plan transportation and follow-up visits Jefferson locations offer varying parking options from garages to surface lots. Ask about shuttle services when you schedule, as some facilities provide transportation assistance for seniors. Plan for weekly or biweekly visits initially, as most wound healing protocols require consistent monitoring and treatment adjustments. Choosing a Jefferson location near public transit or with good parking access reduces the stress of multiple appointments. 4. Temple Health advanced wound care Temple Health operates a wound care
Red Around The Wound: Healing Normal Or Infection Sign?
You notice red around the wound after changing a bandage, and immediately your mind jumps to the worst-case scenario. Is this the start of an infection, or is your body simply doing its job? This question comes up constantly for patients recovering from surgery, managing diabetic ulcers, or caring for aging family members with chronic wounds that require close monitoring. The truth is, some redness is completely expected during the healing process. Your body sends extra blood flow to the injured area, bringing immune cells and nutrients needed for tissue repair. But there’s a clear line between healthy inflammation and the warning signs of something more serious. Knowing the difference can mean the gap between a smooth recovery and a wound that spirals into a dangerous infection. At Philadelphia Wound Care, our physician-led mobile team evaluates wounds like these every day, at bedsides, in skilled nursing facilities, and in patients’ own homes across the Philadelphia area. This article breaks down exactly what to look for, when redness signals trouble, and when it’s time to seek professional wound care rather than waiting it out. Why redness happens during healing Your body launches a complex biological response the moment your skin breaks, and redness is one of the first visible signs that this process has started. Within minutes of injury, your immune system recognizes damage and triggers what clinicians call the inflammatory phase of wound healing. This reaction isn’t a malfunction; it’s your body mobilizing resources to prevent infection and start repairs. Your body’s inflammatory response in action When tissue damage occurs, your cells release chemical messengers called cytokines and histamines that act like an emergency broadcast system. These signals tell your immune system exactly where help is needed. White blood cells rush to the site to fight off bacteria and clear away dead tissue, while platelets work to stop bleeding. This surge of cellular activity generates heat and causes the localized swelling and warmth you often feel around a fresh wound, even if infection isn’t present. Visual characteristics of healthy inflammation Healthy redness looks smooth and even in tone, ranging from bright pink to light red during the first 48 to 72 hours. Your skin maintains its normal texture without developing a shiny, tight appearance that signals excessive swelling. The color intensity peaks within the first two to three days, then steadily lightens as your body transitions from inflammation to tissue repair. Normal healing redness fades progressively, not suddenly or in unpredictable patterns. How it should feel to the touch When you gently touch the area, you’ll notice mild warmth that matches your body’s natural inflammatory response. The skin feels slightly tender but not intensely painful with light pressure. Your wound site may feel somewhat firm due to tissue swelling, but this firmness shouldn’t feel rock-hard or increasingly tight as days pass. Any discomfort remains manageable with over-the-counter pain relief and doesn’t interfere with basic daily activities. When redness signals infection or complications.